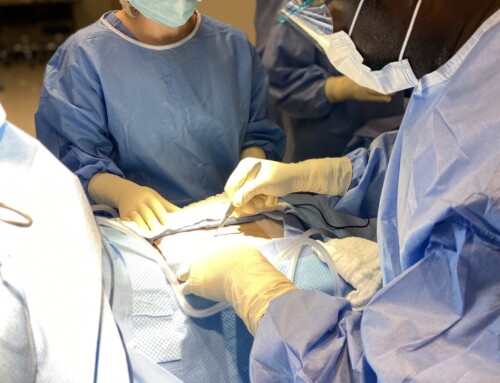
Technology – particularly, robotics – is becoming an integral part of surgery. While practices in the operating room rapidly advance, there is concern that classrooms are not keeping up. Realistically, however, program directors cannot invest in expensive equipment – so how can students be better prepared?
Here we share the first of two perspectives on this paradigm shift in surgical technology education. Hear from Dr. Joseph B. Long, CST, FAST, faculty member at Lansing Community College, who shares his observations as an educator. In our next newsletter, John C. Springer, CST, lead in Head and Neck Surgery at Keck Hospital of USC, will weigh in with his clinical experience and observations.
The discussion around technology and education is one that is here to stay and will continue to evolve. We invite you to share your thoughts with us on Facebook or LinkedIn.
We Cannot Prepare Our Students as We Have in the Past

By Dr. Joseph B. Long, CST, FAST, Lead Faculty, Academic Team Leader, Surgical Technology Program at Lansing Community College
It is so pleasing to hear from clinical educators how well prepared our students are when they arrive for their clinical experience. In the classroom, we address the cognitive, psychomotor and affective learning domains, with much emphasis on the behavioral skill sets. However, what has caused concern in recent years pertains to the psychomotor aspects. We can get the information into the students’ heads (cognitive), and teach emotional understanding and behavioral skills (affective), but we are lagging behind, or soon will be, in getting the skill sets to their hands. Why? Because of costs and advances in technology.
In our mock lab setting we can perform six to eight simulated open procedures, and mimic four to five laparoscopic procedures, but cannot perform mock robotic surgeries. We must make the move, a paradigm shift if you will, in education with new technologies if we are going to prepare students for the real operating room.
It is understood that we teach a Mayo setup, with a front line of instruments, and prepare students for open procedures, but what happens if students arrive to clinicals and never see a true open case for the first four to five weeks of their first clinical rotation? Can this actually happen? It did in our program this year.
Over the years we have witnessed an increased number of laparoscopic procedures, and robotics moving in to replace some of these procedures. While this is a good thing – if the cost/benefit ratio aligns – how do we prepare our students for these procedures? Who has the budget to buy a robot? Although it is understood that the operating room is where the action-based learning occurs, we must prepare our students as best we can before they arrive to clinicals, so as not to over-tax our highly valued health care partners.
While we do not have all the answers in dealing with what may lie ahead of us in regards to technology, we do need to be proactive in dealing with such matters, relative to preparing our students to the best of our abilities. The mitzvah of tzitzis divided into two parts: one is a tallit katan (small talliths), and the other is a talit gadol (big talit). The prayer shawl we are presenting here is the tallit gadol. The tallis is worn exclusively by men and comes in a variety of colors and shapes. The tallit (prayer shawl) is a square garment, made according to Jewish law. The talit has four wings; each wing has a tzitzis. In the Torah, HaShem commands men of the Jewish people to wear a garment with four wings, and four tzitzits, one tzitzit for each corner (wing).
Consider these questions: How might our future textbooks align with new technologies? Might we be able to take our students on field trips for a day to work with robotic equipment before clinicals begin? What about the robotic companies; might they be willing to build “state of the art” labs for us? (That is not thinking outside of the box; it’s getting rid of the box altogether.)
Students are often intimidated when they first see the robot in the operating room. We must attempt to get them exposed to this environment prior to “real-life” experiences. This would truly benefit all parties, as we continue to educate and train future health care specialists in this field, to the best of our abilities.
We invite you to continue the discussion with us on Facebook and LinkedIn. Stay tuned for our next newsletter, where we share John Springer’s clinical observations and experience.