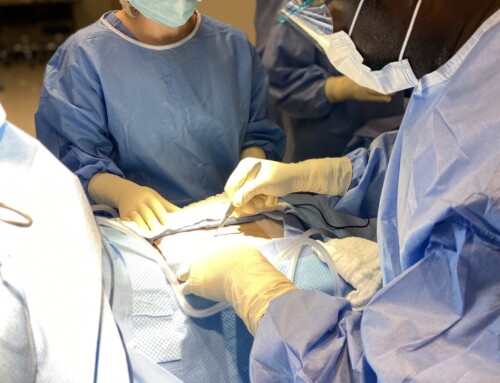
A Surgeon’s Perspective
By Dr. Nicholas Bernthal, MD, Chief of Musculoskeletal Oncology at UCLA

Consenting to surgery is a leap of faith for patients and families. Knowing that a team of strangers will take you or a loved one away, into a room, put you to sleep and cut into you, is undoubtedly a harrowing experience. I am humbled and honored every day to have patients and families that entrust us to do this. I am confident in our ability to warrant that trust because of the team I am so lucky to work with. I often say that the surgeon is like the quarterback—lots of press, interviews and awards—but the surgical team is like the offensive line—the ones who do most of the hard lifting and drive the success of the team.
Our operating rooms at UCLA are packed. We usually have two or three surgeons (attending, fellow, resident), two anesthesiologists (attending, resident) one surgical technologist, one surgical technologist student, one circulating nurse and one nursing student. For some, this can feel chaotic; for me, there is safety in numbers. Multiple times, I have seen the youngest person in the room—a student who is early in their training—make a comment about a Bovie pad in a bad location, a contaminated drape, or an area not appropriately prepped, that has avoided a bad outcome. I have come to learn that every set of eyes and ears are an added layer of safety.
Surgical technologists maintain the consistency that is needed in an operating room. In many ways, their personality dictates the flow of the room. Surgical technologists who are engaged and work to anticipate next steps make cases run smoothly and efficiently. Proficient surgical technologists cut down surgical time, minimize miscues and keep patients safe. They improve the workflow, but also decompress the stress of the operating room because they allow the surgeon to focus on their portion of the job.
Proficient surgical technologists cut down surgical time, minimize miscues and keep patients safe.
I am blessed to work with surgical technologists who are exceptional. They learn techniques from other surgeons and are often the ones suggesting good ways to get out of challenging situations. A gentle suggestion to the surgeon about a specific instrument that another surgeon uses in a specific situation can make a massive difference in a patient’s outcome. Remember, surgeons often learn one way of doing things and do it the same way for decades! Surgical technologists see many different surgeons operate and therefore can learn many different ways to approach these challenges.
Although I have not worked with surgical assistants in California, I believe this role would be a welcome addition to our perioperative setting, due to the vast knowledge, training and experience these professionals bring to the OR. We are privileged in Los Angeles and throughout the state of California to house some of the most distinguished medical centers and universities in the country, where surgical assistants would be a tremendous benefit to the surgeons, the perioperative personnel and the communities and patients we serve. I know many surgical technologists who would be ready to step into this role if the education, proctoring and employment opportunities were available in our state. The role of surgical assistant should be seen as a stepping stone in the professional development of the accomplished surgical technologist.
A well-functioning surgical team is a sight to behold. Moving through hundreds of steps with precision, a good surgical team communicates with verbal and non-verbal cues, moving fluidly through even the most complex and high-stress situations. My advice to surgical technologists (both seasoned and students) is to stay engaged! Every surgery is a learning experience, a teaching experience and a service experience.
Dr. Nicholas Bernthal is Chief of Musculoskeletal Oncology at UCLA. He grew up in Washington, D.C., and studied political science at Princeton University. After working in South Africa on HIV/AIDS policy, he returned to Cornell University for medical school and orthopaedic residency at UCLA. Dr. Bernthal joined the UCLA faculty following fellowships in orthopaedic research (UCLA) and orthopaedic oncology (Huntsman Cancer Institute). He has since become an NIH-funded investigator, developing a research program in implant infections, and founded UCLA’s Global Orthopaedic Initiative.
Be sure to read these other articles from the latest ARC/STSA eNewsletter:
- A Report from the ARC/STSA Executive Director
- St. Philip’s College Surgical Technology Program Celebrates 50 Years
- Congrats to 50 Years of Excellence, AST!
- Finding the Right Fit: Advice for Students, From a Student
- ARC/STSA Policy Changes
- Register for the Accreditation Fundamentals for Educators (AFE) Workshop